Rates have fallen 62{a5554ed3202f5d83946c2df2be5f385c2dbdb5a74c027274cb45634d87826b1f} in women offered the HPV jab between the age of 14 and 16, and 34{a5554ed3202f5d83946c2df2be5f385c2dbdb5a74c027274cb45634d87826b1f} for older teenagers
The NHS vaccination programme to prevent cervical cancer has so far stopped thousands of women from developing the disease and experiencing pre-cancerous changes to cells, a study has found. In the first proof that the programme launched in England 13 years ago is saving lives, the Cancer Research UK-funded study found that cervical cancer rates in women offered the vaccine between the ages of 12 and 13 (now in their 20s) were 87{a5554ed3202f5d83946c2df2be5f385c2dbdb5a74c027274cb45634d87826b1f} lower than in an unvaccinated population.
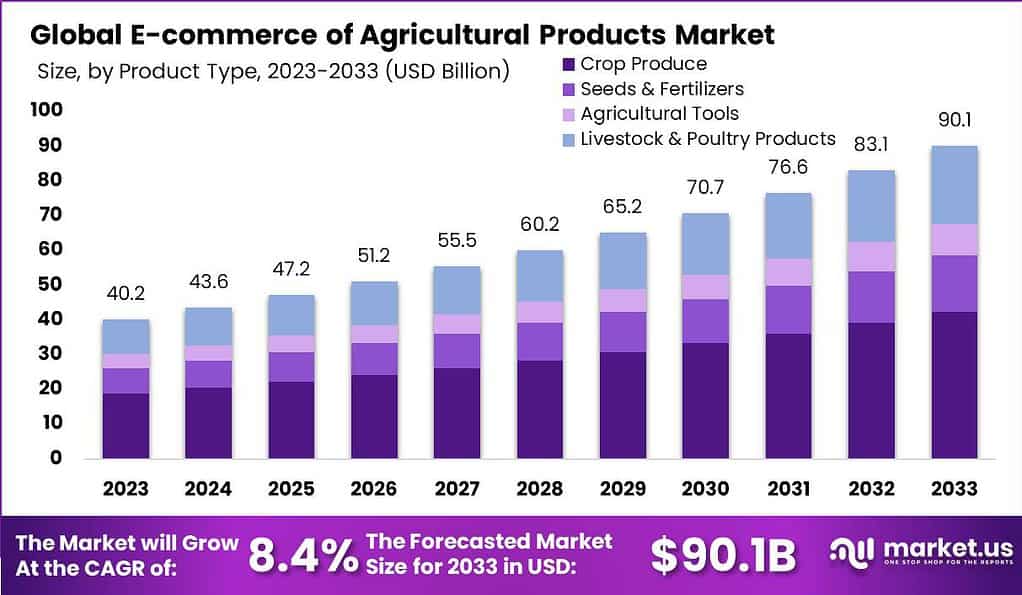
Researchers said cases in this age group, which are rare, dropped from about 50 per year to just five. There were also reductions in cervical cancer rates of 62{a5554ed3202f5d83946c2df2be5f385c2dbdb5a74c027274cb45634d87826b1f} in women offered vaccination between the ages of 14 and 16, and 34{a5554ed3202f5d83946c2df2be5f385c2dbdb5a74c027274cb45634d87826b1f} in women aged 16 to 18 when vaccination was introduced. Experts looked at data from the human papillomavirus (HPV) immunisation programme using the vaccine Cervarix, which was given to girls on the NHS from 2008 to September 2012.
A different vaccine, Gardasil, is now used for the programme, and is given to girls and boys aged 12 and 13. The new study – published in the Lancet on Thursday – was able to use data to estimate that, by June 2019, there were around 450 fewer cases of cervical cancer (down to 374 cases in 2016-2018) and 17,200 fewer cases of cervical carcinomas (pre-cancers) than expected in those vaccinated against HPV in England. The study found a 97{a5554ed3202f5d83946c2df2be5f385c2dbdb5a74c027274cb45634d87826b1f} drop in pre-cancerous changes to cells in women vaccinated between the ages of 12 and 13, 75{a5554ed3202f5d83946c2df2be5f385c2dbdb5a74c027274cb45634d87826b1f} in women vaccinated between the ages of 14 and 16, and 39{a5554ed3202f5d83946c2df2be5f385c2dbdb5a74c027274cb45634d87826b1f} in women vaccinated between the ages of 16 and 18.
Without vaccination, experts believe the toll for pre-cancerous changes could have affected almost 36,000 women. The researchers said the findings provide the first direct, worldwide evidence of prevention of cervical cancer using a vaccine for two types of HPV, which is the virus that causes it.
ABOUT AUTHOR
Devoted my whole life to words - reading, writing and trying to be original on social media. Got certified in digital marketing - still not cool enough to be an influencer. Finished a master’s degree focused in Literature, Publishing, Mass Media. Hobbies include traveling, reading and hoping that yoga will be the thing to finally teach me some patience. Would like to take over the world at some point, but that’s an optional dream. Maybe modern tech can help me do that?